Search results for: 'blog lacusc students and staff use simulation based training to improve covid 19 readiness'
-
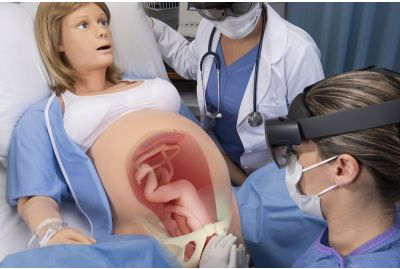 Obstetric MR™ - Mixed Reality Training SystemOBMRLearn More
Obstetric MR™ - Mixed Reality Training SystemOBMRLearn MoreObstetric MR™ is a next-generation mixed reality training solution for VICTORIA® S2200 designed to help learners bridge the gap between theory and practice faster than ever before. Using the latest technology in holographic visualization, Obstetric MR™ brings digital learning content into the physical simulation exercise, allowing participants to link knowledge and skill through an entirely new hands-on training experience. The future of labor and delivery simulation is here.
-
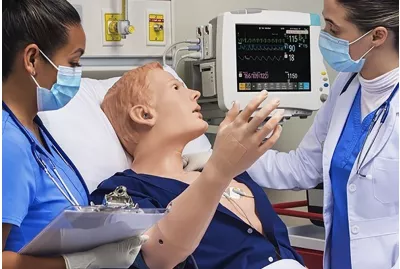 HAL® S5301 - Interdisciplinary and ImmersiveS5301.PKLearn More
HAL® S5301 - Interdisciplinary and ImmersiveS5301.PKLearn MoreMeet the most advanced interdisciplinary patient simulator in the world. From emergency care to ICU and med-surg training, HAL is engineered to fulfill educational objectives across clinical disciplines and blur the lines between simulation and real life. New conversational speech, lifelike motor movement, next-gen simulated physiology, UNI® 3, and many more industry-first capabilities usher in the next revolutionary leap in simulation.
-
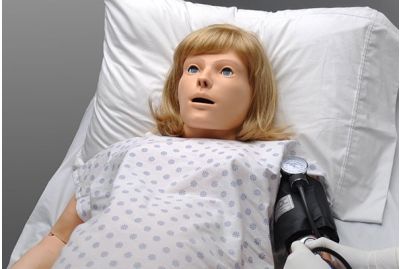 NOELLE® S574.100 - Advanced Maternal Care Simulation PackageS574.100.PKLearn More
NOELLE® S574.100 - Advanced Maternal Care Simulation PackageS574.100.PKLearn MoreThe NOELLE® Advanced Maternal Care package is a complete simulation-based obstetric care education and training solution. This turnkey solution includes a NOELLE® wireless and tetherless childbirth patient simulator, the UNI® control tablet PCs, a Gaumard Vitals® patient monitor, the Labor & Delivery Simulation Learning Experience® Courseware package, and accessories.
-
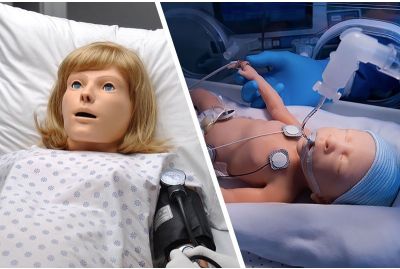 NOELLE® with Premie HAL® S576.100 - Advanced Maternal and Premature Infant Care Simulation PackageS576.100.PKLearn More
NOELLE® with Premie HAL® S576.100 - Advanced Maternal and Premature Infant Care Simulation PackageS576.100.PKLearn MoreThe NOELLE and Premie HAL package is a complete simulation-based obstetric and premature infant care education and training solution for one great price. This turnkey solution includes a Noelle wireless and tetherless childbirth patient simulator, a Premie HAL wireless and tetherless premature infant, two UNI® control tablet PCs, a Gaumard Vitals® patient monitor, Labor & Delivery and Premature Infant Care Simulation Learning Experience® Courseware packages, and accessories.
-
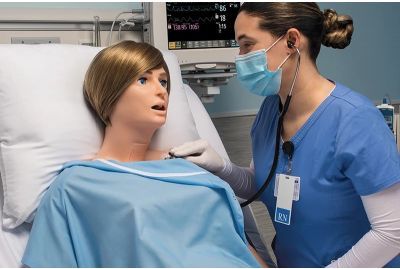 SUSIE® S2400 - Comprehensive Patient Care SimulatorS2400.PKYour all-in-one simulation solution for comprehensive patient care training SUSIE® S2400 is a powerful and versatile training solution specifically designed to streamline high-quality simulation across nursing, allied health, and medicine. Featuring advanced clinical features and the new UNI® 3 control software, SUSIE S2400 enables immersive procedural and scenario-driven exercises using a single platform. This helps simplify your workflow and broaden your program's reach. Learn More
SUSIE® S2400 - Comprehensive Patient Care SimulatorS2400.PKYour all-in-one simulation solution for comprehensive patient care training SUSIE® S2400 is a powerful and versatile training solution specifically designed to streamline high-quality simulation across nursing, allied health, and medicine. Featuring advanced clinical features and the new UNI® 3 control software, SUSIE S2400 enables immersive procedural and scenario-driven exercises using a single platform. This helps simplify your workflow and broaden your program's reach. Learn More -
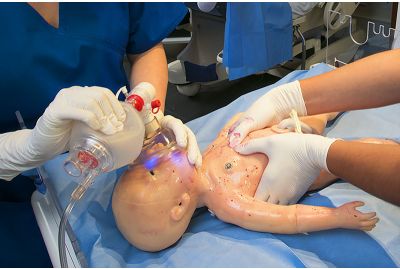 Newborn TORY® S2210 - Wireless and Tetherless Full-term Neonatal Care Patient SimulatorS2210.PKLearn More
Newborn TORY® S2210 - Wireless and Tetherless Full-term Neonatal Care Patient SimulatorS2210.PKLearn MoreNewborn TORY® offers a new level of fidelity with true-to-life physical and physiological attributes essential for effective neonatal care simulation training. With a truly wireless and tetherless design educators can freely simulate clinical cases in any setting, even in transit. Whether in a simulation center or in-situ, Tory brings neonatal simulation closer to real life than ever before.
-
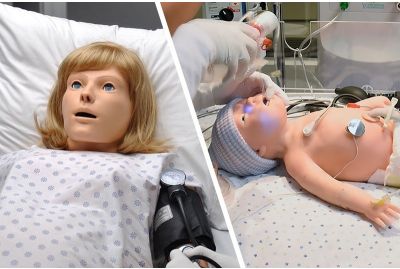 NOELLE® with Newborn TORY® S575.100 - Advanced Maternal and Neonatal Care Simulation PackageS575.100.PKLearn More
NOELLE® with Newborn TORY® S575.100 - Advanced Maternal and Neonatal Care Simulation PackageS575.100.PKLearn MoreThe NOELLE and Newborn TORY package is a complete simulation-based obstetric and neonatal care education and training solution for one great price. This turnkey solution includes a NOELLE wireless and tetherless childbirth patient simulator, a Newborn TORY wireless and tetherless full-term neonate, two UNI® control tablet PCs, a Gaumard Vitals® patient monitor, Labor & Delivery and Neonatal Care Simulation Learning Experience® Courseware packages, and accessories.
-
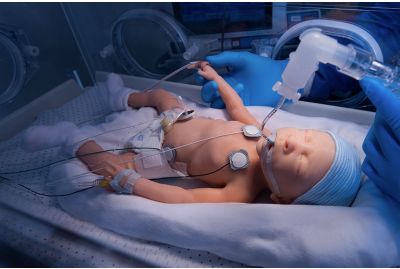 Premie HAL® S2209 30-Week Premature Infant Patient SimulatorS2209.PKLearn MoreLifelike, Wireless and Tetherless Preterm Patient Simulator.The Premie HAL® S2209 is a lifelike, wireless and tetherless 30-week preterm patient simulator designed to facilitate the training of residents and health care professionals in the areas of preterm airway management, resuscitation, stabilization, transport, and intensive care.
Premie HAL® S2209 30-Week Premature Infant Patient SimulatorS2209.PKLearn MoreLifelike, Wireless and Tetherless Preterm Patient Simulator.The Premie HAL® S2209 is a lifelike, wireless and tetherless 30-week preterm patient simulator designed to facilitate the training of residents and health care professionals in the areas of preterm airway management, resuscitation, stabilization, transport, and intensive care. -
 Gaumard Vitals™ Bedside Virtual Patient Monitor for Gaumard PatientsGaumard Vitals BedsideLearn More
Gaumard Vitals™ Bedside Virtual Patient Monitor for Gaumard PatientsGaumard Vitals BedsideLearn MoreThe Gaumard Vitals™ Bedside Patient Monitor offers participants the functionality and versatility of a bedside patient monitor. Participants can practice vital sign documentation and interpretation skills with Gaumard patient simulators and skills trainers in a simulated OR, ICU, or patient room. Compatible with both UNI® and OMNI® 2, the Bedside Patient Monitor helps you create immersive scenarios to enhance simulation-based learning.
-
 Gaumard Vitals™ Portable Virtual Patient Monitor for Gaumard PatientsGaumard Vitals PortableLearn More
Gaumard Vitals™ Portable Virtual Patient Monitor for Gaumard PatientsGaumard Vitals PortableLearn MoreThe Gaumard Vitals™ Portable Patient Monitor offers participants the functionality and versatility of a wireless transport patient monitor. Participants can practice vital sign documentation and interpretation skills with Gaumard patient simulators and skills trainers at the bedside, in transit, or in the field. Compatible with both UNI® and OMNI® 2, the Portable Patient Monitor helps you create immersive scenarios to enhance simulation-based learning.
