Search results for: 'blog why america needs more midwives'
-
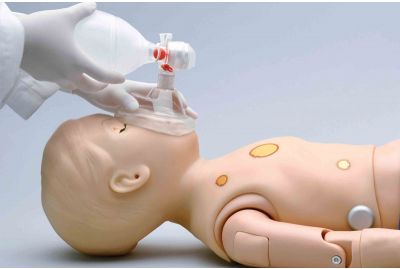 Pediatric HAL® S3004 - Wireless and Tetherless, One-Year-Old Patient SimulatorS3004.PKLearn More
Pediatric HAL® S3004 - Wireless and Tetherless, One-Year-Old Patient SimulatorS3004.PKLearn MorePediatric HAL® is a high-fidelity toddler patient simulator specifically designed to meet the needs of pediatric care training programs. Pediatric HAL can help your care teams improve teamwork and patient care through hands-on scenario-based training. Participants can practice and develop airway management, auscultation, ventilation, CPR, IV/IO placement skills, and more.
-
 Trauma HAL® S3040.50 - Wireless and Tetherless Trauma Care Patient SimulatorS3040.50.PKLearn MoreThe Trauma HAL® S3040.50 is a wireless and tetherless full-body trauma patient simulator featuring bleeding, pressure-sensitive wounds and trauma limbs, laryngospasms, spontaneous chest rise, bilateral intravenous training arms, and many more capabilities. The completely tetherless design and ruggedized joints make this simulator perfect for point of injury, care under fire, emergency field care, extraction, patient transport, mass casualty, decontamination, and more.
Trauma HAL® S3040.50 - Wireless and Tetherless Trauma Care Patient SimulatorS3040.50.PKLearn MoreThe Trauma HAL® S3040.50 is a wireless and tetherless full-body trauma patient simulator featuring bleeding, pressure-sensitive wounds and trauma limbs, laryngospasms, spontaneous chest rise, bilateral intravenous training arms, and many more capabilities. The completely tetherless design and ruggedized joints make this simulator perfect for point of injury, care under fire, emergency field care, extraction, patient transport, mass casualty, decontamination, and more. -
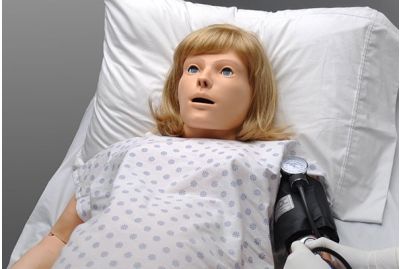 NOELLE® S574.100 - Advanced Maternal Care Simulation PackageS574.100.PKLearn More
NOELLE® S574.100 - Advanced Maternal Care Simulation PackageS574.100.PKLearn MoreThe NOELLE® Advanced Maternal Care package is a complete simulation-based obstetric care education and training solution. This turnkey solution includes a NOELLE® wireless and tetherless childbirth patient simulator, the UNI® control tablet PCs, a Gaumard Vitals® patient monitor, the Labor & Delivery Simulation Learning Experience® Courseware package, and accessories.
-
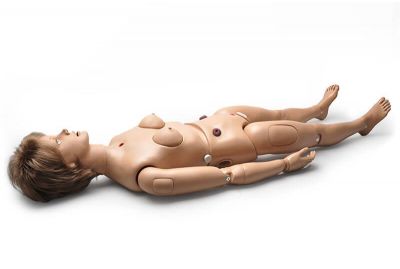 Clinical CHLOE™ S221 - Original Nursing Care Patient SimulatorS221.PKLearn More
Clinical CHLOE™ S221 - Original Nursing Care Patient SimulatorS221.PKLearn MoreClinical CHLOE™ S221 is a full-body, adult-sized simulator designed for wireless training of general nursing skills, including tracheostomy procedures, bandaging, breast examinations, and more.
-
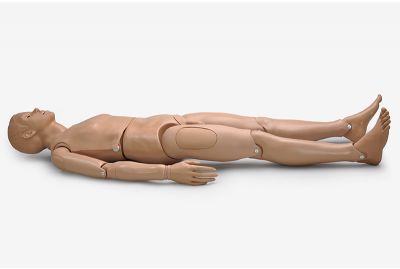 Simple Simon® S205 - Nursing Care Patient SimulatorS205.PKLearn MoreThe Simple Simon® Nursing Care Patient Simulator is a full-body, adult-sized manikin designed for the simulation-based training of general nursing clinical skills. The S205 allows participants to work hands-on and hone tracheostomy care, bandaging, ophthalmic exercises, and other nursing care skills.
Simple Simon® S205 - Nursing Care Patient SimulatorS205.PKLearn MoreThe Simple Simon® Nursing Care Patient Simulator is a full-body, adult-sized manikin designed for the simulation-based training of general nursing clinical skills. The S205 allows participants to work hands-on and hone tracheostomy care, bandaging, ophthalmic exercises, and other nursing care skills. -
 S200 Susie Simon® Patient Care Simulator (without Ostomy)S200.PKLearn More
S200 Susie Simon® Patient Care Simulator (without Ostomy)S200.PKLearn MoreThe S200 Susie Simon® Patient Care Simulator is an adult manikin designed for the simulation-based training of general nursing clinical skills, including IV training, trach care, catheterization, enema, nasogastric feeding, bandaging, and more.
-
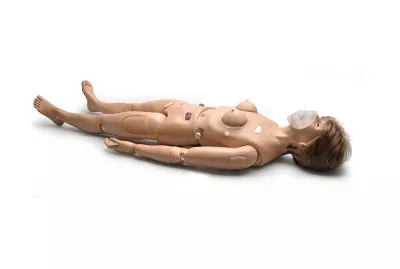 Code Blue® S304 - Multipurpose Patient Simulator with Disposable AirwayS304.PKLearn MoreThe Code Blue® S304 is a full-body, adult-sized patient simulator designed for the hands-on training of general nursing and BLS skills, including ostomy care, breast examination, injection and infusion techniques, CPR, and more.
Code Blue® S304 - Multipurpose Patient Simulator with Disposable AirwayS304.PKLearn MoreThe Code Blue® S304 is a full-body, adult-sized patient simulator designed for the hands-on training of general nursing and BLS skills, including ostomy care, breast examination, injection and infusion techniques, CPR, and more. -
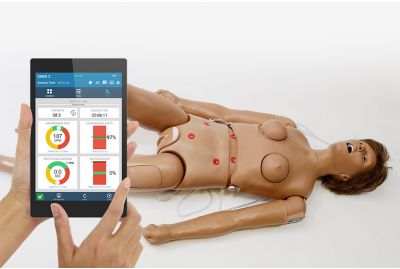 Clinical CHLOE™ S222 - Nursing Care Patient Simulator with OMNI® 2S222.250.PKLearn More
Clinical CHLOE™ S222 - Nursing Care Patient Simulator with OMNI® 2S222.250.PKLearn MoreClinical CHLOE™ Nursing Care Patient Simulator with OMNI® 2 is a full-body, adult-sized simulator with wireless control designed for training general nursing clinical skills. Participants can work hands-on and develop skills in CPR, tracheostomy procedures, bandaging, breast examinations, and more.
-
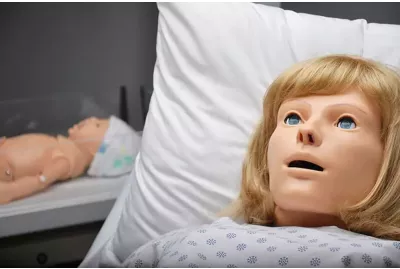 NOELLE® with Newborn S554.100 - Maternal Care and Neonatal Resuscitation Simulation PackageS554.100.PKLearn More
NOELLE® with Newborn S554.100 - Maternal Care and Neonatal Resuscitation Simulation PackageS554.100.PKLearn MoreThe NOELLE® and Newborn package is a complete simulation-based obstetric care and neonatal resuscitation education and training solution. This turnkey solution includes a NOELLE childbirth patient simulator, a full-term newborn, UNI® control Laptop PCs, a Gaumard Vitals® patient monitor, Labor & Delivery Simulation Learning Experience® Courseware package, and accessories.
-
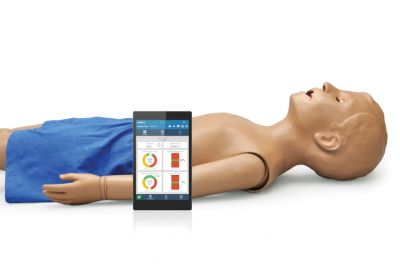 Five-Year-Old Multipurpose Patient Simulator with OMNI® 2 (S157.250)S157.250.PKLearn MoreThe MIKE® and MICHELLE® 5-year-old is a sophisticated pediatric simulator for training standard and advanced clinical procedures and resuscitation skills, including CPR, intubation, trach care, IV access, and more.
Five-Year-Old Multipurpose Patient Simulator with OMNI® 2 (S157.250)S157.250.PKLearn MoreThe MIKE® and MICHELLE® 5-year-old is a sophisticated pediatric simulator for training standard and advanced clinical procedures and resuscitation skills, including CPR, intubation, trach care, IV access, and more.
