Search results for: 'blog unh paramedics use simulation for hands on childbirth training'
-
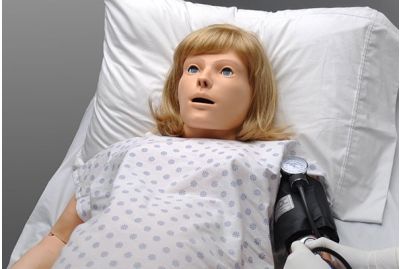 NOELLE® S574.100 - Advanced Maternal Care Simulation PackageS574.100.PKLearn More
NOELLE® S574.100 - Advanced Maternal Care Simulation PackageS574.100.PKLearn MoreThe NOELLE® Advanced Maternal Care package is a complete simulation-based obstetric care education and training solution. This turnkey solution includes a NOELLE® wireless and tetherless childbirth patient simulator, the UNI® control tablet PCs, a Gaumard Vitals® patient monitor, the Labor & Delivery Simulation Learning Experience® Courseware package, and accessories.
-
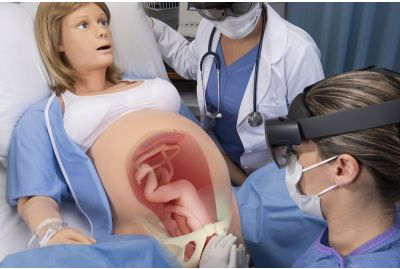 Obstetric MR™ - Mixed Reality Training SystemOBMRLearn More
Obstetric MR™ - Mixed Reality Training SystemOBMRLearn MoreObstetric MR™ is a next-generation mixed reality training solution for VICTORIA® S2200 designed to help learners bridge the gap between theory and practice faster than ever before. Using the latest technology in holographic visualization, Obstetric MR™ brings digital learning content into the physical simulation exercise, allowing participants to link knowledge and skill through an entirely new hands-on training experience. The future of labor and delivery simulation is here.
-
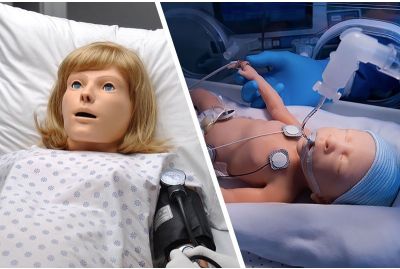 NOELLE® with Premie HAL® S576.100 - Advanced Maternal and Premature Infant Care Simulation PackageS576.100.PKLearn More
NOELLE® with Premie HAL® S576.100 - Advanced Maternal and Premature Infant Care Simulation PackageS576.100.PKLearn MoreThe NOELLE and Premie HAL package is a complete simulation-based obstetric and premature infant care education and training solution for one great price. This turnkey solution includes a Noelle wireless and tetherless childbirth patient simulator, a Premie HAL wireless and tetherless premature infant, two UNI® control tablet PCs, a Gaumard Vitals® patient monitor, Labor & Delivery and Premature Infant Care Simulation Learning Experience® Courseware packages, and accessories.
-
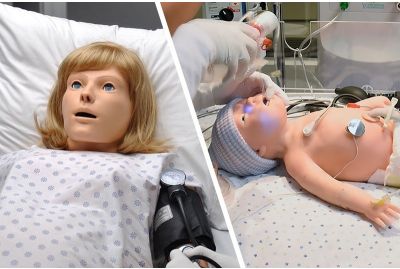 NOELLE® with Newborn TORY® S575.100 - Advanced Maternal and Neonatal Care Simulation PackageS575.100.PKLearn More
NOELLE® with Newborn TORY® S575.100 - Advanced Maternal and Neonatal Care Simulation PackageS575.100.PKLearn MoreThe NOELLE and Newborn TORY package is a complete simulation-based obstetric and neonatal care education and training solution for one great price. This turnkey solution includes a NOELLE wireless and tetherless childbirth patient simulator, a Newborn TORY wireless and tetherless full-term neonate, two UNI® control tablet PCs, a Gaumard Vitals® patient monitor, Labor & Delivery and Neonatal Care Simulation Learning Experience® Courseware packages, and accessories.
-
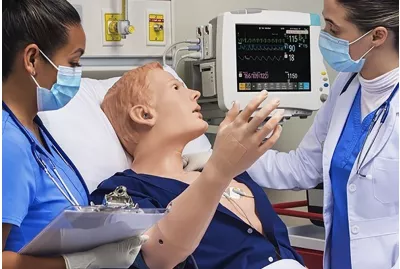 HAL® S5301 - Interdisciplinary and ImmersiveS5301.PKLearn More
HAL® S5301 - Interdisciplinary and ImmersiveS5301.PKLearn MoreMeet the most advanced interdisciplinary patient simulator in the world. From emergency care to ICU and med-surg training, HAL is engineered to fulfill educational objectives across clinical disciplines and blur the lines between simulation and real life. New conversational speech, lifelike motor movement, next-gen simulated physiology, UNI® 3, and many more industry-first capabilities usher in the next revolutionary leap in simulation.
-
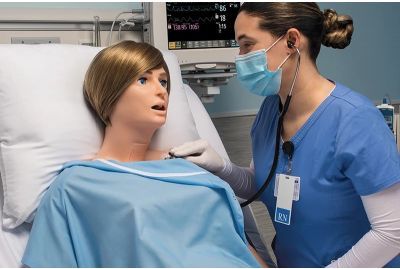 SUSIE® S2400 - Comprehensive Patient Care SimulatorS2400.PKYour all-in-one simulation solution for comprehensive patient care training SUSIE® S2400 is a powerful and versatile training solution specifically designed to streamline high-quality simulation across nursing, allied health, and medicine. Featuring advanced clinical features and the new UNI® 3 control software, SUSIE S2400 enables immersive procedural and scenario-driven exercises using a single platform. This helps simplify your workflow and broaden your program's reach. Learn More
SUSIE® S2400 - Comprehensive Patient Care SimulatorS2400.PKYour all-in-one simulation solution for comprehensive patient care training SUSIE® S2400 is a powerful and versatile training solution specifically designed to streamline high-quality simulation across nursing, allied health, and medicine. Featuring advanced clinical features and the new UNI® 3 control software, SUSIE S2400 enables immersive procedural and scenario-driven exercises using a single platform. This helps simplify your workflow and broaden your program's reach. Learn More -
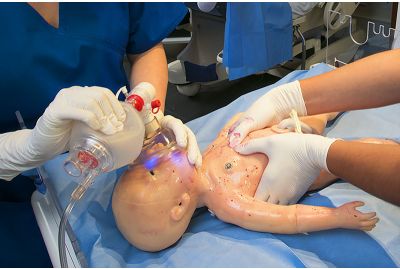 Newborn TORY® S2210 - Wireless and Tetherless Full-term Neonatal Care Patient SimulatorS2210.PKLearn More
Newborn TORY® S2210 - Wireless and Tetherless Full-term Neonatal Care Patient SimulatorS2210.PKLearn MoreNewborn TORY® offers a new level of fidelity with true-to-life physical and physiological attributes essential for effective neonatal care simulation training. With a truly wireless and tetherless design educators can freely simulate clinical cases in any setting, even in transit. Whether in a simulation center or in-situ, Tory brings neonatal simulation closer to real life than ever before.
-
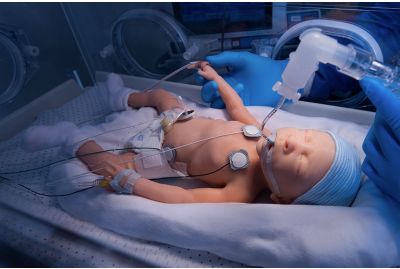 Premie HAL® S2209 30-Week Premature Infant Patient SimulatorS2209.PKLearn MoreLifelike, Wireless and Tetherless Preterm Patient Simulator.The Premie HAL® S2209 is a lifelike, wireless and tetherless 30-week preterm patient simulator designed to facilitate the training of residents and health care professionals in the areas of preterm airway management, resuscitation, stabilization, transport, and intensive care.
Premie HAL® S2209 30-Week Premature Infant Patient SimulatorS2209.PKLearn MoreLifelike, Wireless and Tetherless Preterm Patient Simulator.The Premie HAL® S2209 is a lifelike, wireless and tetherless 30-week preterm patient simulator designed to facilitate the training of residents and health care professionals in the areas of preterm airway management, resuscitation, stabilization, transport, and intensive care. -
 VICTORIA® S2200 - Wireless and Tetherless, Maternal and Neonatal Care Patient SimulatorS2200.PKLearn More
VICTORIA® S2200 - Wireless and Tetherless, Maternal and Neonatal Care Patient SimulatorS2200.PKLearn MoreFrom early pregnancy complications, high-risk deliveries, and postpartum emergencies to non-gravid scenarios for general nursing care, Victoria simulates a full range of obstetrical events to facilitate teamwork and deepen critical thinking skills in learners of all levels.
More than a childbirth simulator, Victoria is a complete simulation solution
developed from decades of obstetrical experience. It is a comprehensive package of tools and support designed to help improve patient safety in women’s health through education and training.
-
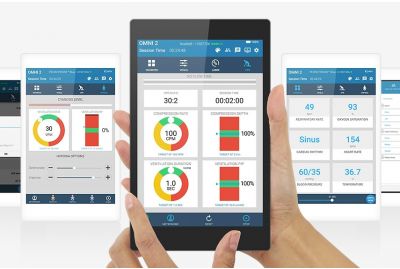 OMNI® 2 Controlling, Monitoring & Debriefing. Simulation Made Easy™OMNI2Learn MoreOMNI® 2 makes it easier than ever to drive scenarios, monitor performance, and capture participants' actions for data-rich debriefing sessions. OMNI® 2 is simple to operate with touchscreen controls and an intuitive layout that lets you manage physiological changes while remaining focused on the training. Put simply, it's a frustration-free solution that works to complement your clinical know-how.
OMNI® 2 Controlling, Monitoring & Debriefing. Simulation Made Easy™OMNI2Learn MoreOMNI® 2 makes it easier than ever to drive scenarios, monitor performance, and capture participants' actions for data-rich debriefing sessions. OMNI® 2 is simple to operate with touchscreen controls and an intuitive layout that lets you manage physiological changes while remaining focused on the training. Put simply, it's a frustration-free solution that works to complement your clinical know-how.
